
Medical School
Baylor College of Medicine
Fellowship
Spine Fellowship at Orthopedic Indianapolis
Internship & Residency
Southern Illinois University School of Medicine
Office Hours
Monday through Friday 8:00 am to 5:00 pm
Make an Appointment
Dr. Rutz’s Philosophy
 I am a Board-Certified Orthopedic Surgeon who sub-specializes in spinal surgery. When I came into practice in 2003, my goal was to become a Physician who was completely specialized in spinal surgery only. By 2005, I no longer performed general orthopedic surgery; meaning that I no longer performed hip, knee, shoulder, hand or foot surgery. My practice is completely dedicated to the operative and nonoperative treatment of the cervical, thoracic and lumbar spine. By performing a large volume of spinal procedures, I have the benefit of experience. I believe this experience has helped me avoid complications and determine who surgical intervention will help and who it will not.
I am a Board-Certified Orthopedic Surgeon who sub-specializes in spinal surgery. When I came into practice in 2003, my goal was to become a Physician who was completely specialized in spinal surgery only. By 2005, I no longer performed general orthopedic surgery; meaning that I no longer performed hip, knee, shoulder, hand or foot surgery. My practice is completely dedicated to the operative and nonoperative treatment of the cervical, thoracic and lumbar spine. By performing a large volume of spinal procedures, I have the benefit of experience. I believe this experience has helped me avoid complications and determine who surgical intervention will help and who it will not.
In my practice, we commonly perform lumbar microdiscectomies, lumbar fusions, and cervical fusions. Also, for the past 6 years, I have taken a special interest in cervical disc arthroplasties (cervical disc replacements). I have performed over 700 of these disc replacement procedures.
Like many surgeons, I try to select the most effective and least invasive treatment possible, without increasing risk. When my team and I see a new patient in the office, our number one goal is to diagnose the problem that they have and lay forth a treatment plan. The treatment might be as simple as medication or an order for physical therapy. Other times, a patient will present with a problem that we know will not resolve without surgical intervention. Our goal is to explain these options to the patient, so they can make an educated decision about their treatment plan. If we feel long-term, non-operative pain management and long-term narcotic medications are the best treatment option, there are other specialties that are more appropriate for those patients.
Practice Set-Up
Lien Patients/Litigated Cases
Workers’ Compensation Patients
Conditions Treated
Episodes of low back pain are extremely common and 90% of people will have a major episode of back pain in their lifetime. Most episodes of low back pain resolve on their own, within 6 to 12 weeks. If the patient has lower back pain without any symptoms into the legs, then we believe initial treatment does not require spinal surgery consultation. I would generally recommend that the patient ask their Primary Care Physician, for anti-inflammatory or steroid medication to help calm down the inflammation which leads to many episodes of back pain and to consider physical therapy. It is also important for the patient to understand that even though symptoms can be quite severe at first, it can be surprising how much resolution of symptoms happen on their own within a few weeks to a few months.
In patients that have back pain that continues to trend in a negative direction over several months, is intractable, or is persistent for greater than 3 months, I believe it is reasonable to obtain an MRI to try to reach a more definitive diagnosis. In our practice, we do not have one specific timeline for when it is appropriate to get an MRI, as every patient is different. In some people, they clearly do not require an MRI and others should have it performed much sooner than many guidelines recommend. Our goal is to obtain the appropriate imaging when it makes the most sense for the patient. The most important thing in treating chronic back pain is to first come up with the correct diagnosis, as treatment varies markedly depending on the primary cause. The most common causes of chronic lower back pain are arthritis of the joints, lumbar stenosis, and spinal instabilities like lumbar spondylolisthesis or disc degeneration. It is common to have these problems on an MRI Scan without them being the cause of the patient’s symptoms. Thus, there is need for a thorough evaluation to determine the exact origin of symptoms. Once a diagnosis has been obtained, we are in a much better position to determine if surgery is indicated.
The lumbar disc is basically the cushion that sits between the bones of the lumbar spine, which provides stability and shock absorption. Over time, everybody’s discs degenerate to some degree and this is part of normal aging. A disc is made up of several parts, primarily a tough outer part and the soft inner core. A lumbar disc herniation is when the soft inner part pushes through the tough outer part. When the soft inner disc material pushes through the outer part and lands against a nerve, the patient can develop pain in the distribution of that nerve. Disc herniations can occur at any level in the spine but are most common in the lower lumbar spine. When this occurs, patients will often develop pain in the buttock going down into their legs. Many disc herniations improve without surgical intervention, as the natural history of many disc herniations are to improve on their own. Over time, the body can resorb or wall off the disc material that entered the spinal canal, at which time patient quits being symptomatic from it.
Surgical intervention is considered when a patient has a neurologic deficit from the disc herniation or significant discomfort that is failing to improve with nonoperative measures. Different disc herniations have what I would call different personalities; some are quite mild, and others are extremely severe.
When it comes to surgical intervention, most disc herniations can be treated by a procedure known as a lumbar microdiscectomy. This is an out-patient procedure which has the goal of removing the herniated disc material. If a patient’s primary complaint prior to surgery is pain in the buttock and down the leg, the procedure has a very good success rate for relieving this. If a patient has a disc herniation in the central portion of the disc with a primary complaint of back pain, the results of a microdiscectomy are more variable, as some patients with this type disc herniation have pain coming from their disc herniation and others have it coming from structural damage to the disc itself. A lumbar microdiscectomy will not fix back pain from structural damage to the disc. The results of surgery on this type of disc herniation are best determined through a thorough discussion with a surgeon who knows the history of your disc herniation, the history of your back pain, and has reviewed your MRI images.
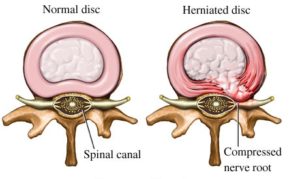
Lumbar radiculopathy is a condition in which a patient develops symptoms from compression or inflammation of a nerve root in the lumbar spine. The most common symptoms are pain, numbness or tingling going through the buttock down into the legs. Some patients will present with weakness of varying degrees. The two most common causes of lumbar radiculopathy are lumbar disc herniations and lumbar stenosis. A large percentage of patients with symptoms from a disc herniation improve without surgical intervention, as many disc herniations can resorb over time. This leads to spontaneous improvement of symptoms. Nonoperative treatment is aimed at controlling symptoms while the body tries to heal itself. A lumbar microdiscectomy is performed for cases that are more severe and fail to have a good response to nonoperative care. Patients that have lumbar radiculopathy from lumbar spinal stenosis are less likely to have resolution of their symptoms with nonoperative care. Lumbar stenosis is caused by degenerative changes, which do not have a natural history of resorption. It should be noted that the patient with lumbar stenosis causing lumbar radiculopathy will at times improve without surgical intervention. Patients that have symptoms for more than 3 months on a consistent or worsening basis, are less likely to have long term resolution of their symptoms without surgical intervention.
Lumbar Spinal Stenosis is a narrowing of the canals in the spine where our nerves travel, most often because of degenerative changes. This narrowing is often the result of bone spurs off the back of the disc or growing off the joints in the back of the spine. Stenosis can lead to compression of the nerves. The ligament that lines the inside of the spinal canal can thicken and also lead to spinal stenosis. The symptoms of spinal stenosis can range from pain, numbness, and/or tingling going down the legs, to symptoms of the legs feeling tired after standing or walking for a few moments and relieved by sitting down. Spinal stenosis is extremely common and much of it is not symptomatic or is only symptomatic when flared up. In these cases, oral medications, physical therapy, and/or epidural steroid injections can be quite helpful. Patients who have had symptoms for greater than 3 months or who have worsening symptoms are much more likely to require surgical intervention.
A lumbar degenerative spondylolisthesis is a common condition in which the joints in the back of the spine wear out. This leads to one bone sliding forward on another bone. As this occurs, this leads to narrowing of the nerve tunnels, which can cause pain into the buttock, and possibly into the legs. The condition can present many different ways. Symptoms may consist of mild back pain from the arthritic component, severe pain in the back, severe pain in the legs, or even weakness in the legs. The best way to understand this condition is to think of it as mild, moderate, or severe. In many ways, it is not that different than knee arthritis. People with mild knee arthritis often respond to physical therapy and an injection and do not need a knee replacement. People with severe degeneration of their knee joint that can only walk 100 feet before they have pain are probably not going to get better until they have a complete knee replacement. It is similar in patients with a lumbar degenerative spondylolisthesis. People with early/mild degeneration often respond to physical therapy, weight loss, core conditioning and possibly epidural steroid injections. People with severe erosion of the joints in the back of their spine with significant instability and 3 months of progressively worsening symptoms are very unlikely to have resolution of their symptoms without surgical intervention. The decision for surgery is based on combining the patient’s history, response to previous treatments and what is found on x-rays and advanced imaging studies. Many patients with this condition require a lumbar fusion for resolution of their symptoms. It is one of the more common reasons a lumbar fusion is performed in the United States.
Lumbar spondylosis is a medical term that simply refers to arthritis, or degeneration of the joints in the lumbar spine. As we age, it is common to see arthritic changes in the lumbar spine and many of these are not significantly symptomatic. Some people will develop more severe degeneration of the joints in their lumbar spine with more consistent symptoms and seek treatment. Maintaining an ideal body weight and keeping your core muscles strong is the first line of treatment and if this is not done, the results of almost any other type of treatment will be quite limited. Physical therapy and daily core exercises are of benefit in some patients. For problems above and beyond that, patients will often see pain management physicians for injections. Our office often refers patients to physicians for evaluation for a rhizotomy (radiofrequency ablation). This is a procedure in which a pain management physician can use a thermal probe to ablate the small nerves that go to the joints in the back of the spine, so that the patient no longer feels the pain from those joints. We do not perform this procedure but often make referrals for it.
The vast majority of arthritis in the lumbar spine does not require surgical intervention. If a patient fails all nonoperative measures and has severe degeneration, surgical intervention can be performed in the form of a lumbar fusion. This will remove the arthritic pain generators from the levels that are operated on.
A lumbar strain is an injury to the muscles or tendons of the lumbar spine secondary to a physical overload of the spine. Lumbar strains should improve on their own over 2 to 3 months. We often see patients who were told that they had a lumbar strain, however, they continued to have symptoms that lasted more than 3 months. In that case, we believe that it is less likely that the primary problem is a pulled muscle or tendon, and more likely some sort of structural injury to another part of the spine. Muscles and tendons would have healed within that time period. In a case of back pain in a patient who was previously told that it was simply a lumbar strain, further diagnostics are required to reach a true diagnosis.
Cervical myelopathy is a pathologic condition in which the patient develops compression of the spinal cord in their cervical spine. It is common to see varying degrees of compression of the spinal cord in the cervical spine. If patients are not symptomatic, we generally do not recommend surgical intervention, as we do not believe that the data supports automatically operating on a spinal cord compression. On the other hand, when a patient presents with symptoms of spinal cord compression (numbness, weakness in the arms or legs, decreased balance, or decreased hand coordination), we strongly recommend surgical intervention. The goal of surgery is to take pressure off the spinal cord and stop the progression of the neurologic loss. There is no guarantee of recovery of neurologic function after surgery. Patients who are treated earlier, often do significantly better. Thus, this is one of the areas of spinal surgery that we will be more aggressive in recommending surgical intervention. It should be noted that compression of the spinal cord is not necessarily a painful condition, which is different than many other spinal conditions.
Many patients say that they are suffering from degenerative disc disease and that they have a family history of it. The term degenerative disc disease is somewhat misleading in that everybody’s discs degenerate as they age. It is normal to have some degree of disc degeneration. What is important to know, is that most degenerated discs are not major pain generators and simply having a degenerated disc does not mean that this is the main cause of the patient’s symptoms. Knowing this, there are a number of people that do have symptomatic disc degeneration. Depending on the severity of symptoms, and lack of successful non-operative care, there are often surgical treatment options.
As we age, everybody develops some degree of degeneration of the discs in their cervical and lumbar spine. This is part of normal aging. Most disc degeneration is painless, or symptoms are relatively mild. There are, however, a subsection of patients who develop chronic neck or back pain that does not respond to physical therapy and/or pain management treatment. In those cases, some surgeons recommend surgical intervention, and some do not. Surgical treatment of cervical and lumbar disc degeneration is a controversial area in spine surgery. We believe in carefully selecting cases in which surgical intervention can be of benefit. However, the majority of degenerating discs do not require surgical intervention.
In general, we do not like the term bulging disc. It is not a good diagnostic term and is ambiguous. Many patients come in telling us that they have bulging discs and that is the source of their pain; however, this is an assumption.
The disc is made up of a softer inner part and a tougher outer part. When we are young, the middle part of the disc is well hydrated, making the discs tall. As we age, the middle of the disc can dehydrate causing loss of height. This causes the outer part of the disc to bow out. Think of a tire that is low on air and how the tire contacting the ground bows out at its edges. The tire itself is fine, it is simply low on air. A bulge of a disc develops because the disc has degenerated to some degree, and the outer part is bowing out.
This bowing out of the disc is significant when it causes narrowing of the nerve tunnels. There typically has to be other degenerative changes, along with the bulging of the disc, to cause compression of the nerves. When this occurs, we refer to it as lumbar spinal stenosis. Many patients have lumbar disc herniations and call them bulging discs, but these are really two different things. A disc herniation is a rupture of disc material through the outer part of the disc, known as the annulus, whereas a bulging disc has an intact annulus. The natural history of a disc herniation in many cases is to improve on its own. Once a disc has degenerated, it will always have a bulge, which is often not symptomatic.
Often a patient will come in telling us that they “broke their tailbone”. If indeed they fractured their sacrum or their coccyx, these bones will heal on their own while being uncomfortable for a few months. When a patient has fallen on their tailbone and has had symptoms for more than 3 months, it is less likely that it is from a fracture of the bone, and more likely that it is from an injury to the joint that connects the coccyx, or tailbone, to the sacrum. Nonoperative care for this consists of physical therapy and injections. Patients who have symptoms that go on for more than 6 months and have failed nonoperative treatment can be evaluated to see if they are a candidate for a coccygectomy. The structure that is causing the persistent pain is the joint, and by removing the coccyx, the painful joint is removed as well. This can be done because we do not need our coccyx or the sacrococcygeal joint. This is different than almost every other joint in the body, in which we need the joint to function properly. A coccygectomy is an outpatient procedure.
Procedures Performed
Cervical disc replacement was approved by the FDA over ten years ago but was not being paid for by insurance companies routinely until the 5-year outcome data from the FDA trials came out. In general, the outcome for these trials looked quite good for cervical disc replacement and insurance companies started routinely approving this procedure. A cervical disc replacement is an alternative to a cervical fusion in many patients. We have found that 70% of the patients that we previously treated with a cervical fusion can now be treated with a cervical disc replacement. We often have patients come in that have been told that a cervical fusion is their only option when, in our opinion, this is not the case, and they are candidates for disc replacement. As of 2020, we have performed over 700 cervical disc replacements. Overall, we are fans of this technology and indeed Dr. Rutz has a cervical disc replacement in his own neck.
Postop Recovery: The cervical disc replacement is performed with an incision on the front of the neck to get to the front of the spine. This is the same approach as is used in a cervical fusion. The difference in the postop recovery is that we generally do not place any restrictions on the patient from the very beginning. Our premise is that the implants are stable from the moment that they are put in; much like a knee replacement is stable from the moment it is performed. Your neck will be sore, however, performing various activities such as lifting, twisting, and bending will not change the ultimate outcome of the procedure. Patients vary in how sore they are after surgery. The average patient will take Ibuprofen 3 times a day until they return to see us for their 2-week follow-up visit. The average patient notes that they needed narcotic pain medication for only a day or two, and then they take only the Ibuprofen. About 20% of patients take no narcotic pain medication after surgery at all. It is normal for patients who have pain down their arm before surgery, to find that it is gone when they wake up. The pain from the surgery itself is referred to the back of the neck and down between the shoulder blades and out over the shoulders. In the average patient, this is 50% better by 2 weeks and 90% better by 6 weeks. It is common for people to have small aches and twinges that are relatively minor but noticeable and these seem to fade away by 6 months. People that do office- type work will often return to work within a week. People that do heavy physical labor might take 6 to 8 weeks because of soreness.
A cervical fusion is a procedure in which the surgeon approaches the cervical spine through the front of the neck. The disc is removed from the level or levels that are pathologic and then appropriate decompression of the spinal cord or nerve roots is performed. This can be done for cervical stenosis and cervical radiculopathy. It has an extremely high success rate for resolving cervical radiculopathy and stopping cervical myelopathy. After the nerves are decompressed, either a bone graft or cage is placed in the disc space and secured with a plate. In our practice, we currently use 3-D printed titanium cages and man-made bone graft and a plate. With this, our fusion rate is over 98% and we do not place our patients in a collar after surgery. We do recommend a 20-pound lifting restriction for approximately 2 months. Once the bones are healed, those levels should no longer be pain generators.
Postop Recovery: An anterior cervical discectomy and fusion procedure in our practice requires an overnight stay. The surgery itself, in our opinion, is an out-patient level procedure except for the rare risk of a postoperative bleed, which occurs in 1 out of 500 patients. Because a postoperative bleed can affect the airway, I have most of my patients spend the night for observation. By the time morning comes, that risk becomes negligible and I feel comfortable discharging them home. After surgery, patients will often complain of a sore throat, feeling like they have a lump in their throat. Some people can be a little hoarse and will notice that they are sore and achy in the back of their neck, down between their shoulder blades, and out over their shoulders. This is the normal referred pattern of discomfort from the procedure, which resolves as they heal. I do not normally place my patients in a neck brace/collar after surgery, as I believe that the implants that we use are adequately stable. It takes 2 to 3 months for the bones in an anterior cervical fusion to heal together and therefore, we recommend a loose 20-pound lifting restriction for a few months after surgery. After the fusion has healed, the patient does not generally have any permanent restrictions.
A lumbar microdiscectomy is an extremely common procedure. A small incision is made, muscles are elevated off the back of the spine, and a small retractor is placed to create a small tunnel through which the surgeon can work to take care of the problem. A small amount of bone is removed from the spine in order to gain access to the spinal canal. The nerves are identified and carefully moved to the side so that the disc material that has ruptured up against the nerves can be removed. Once the nerve compression is relieved, the wound is closed with absorbable sutures and in our practice, we often use skin glue for the outer layer to seal the wound. During the procedure, local anesthetic is placed in the skin and muscles, so many patients wake up without surgical pain for at least 8 to 24 hours. In most of our patients, we prescribe Ibuprofen or some other anti-inflammatory for postoperative pain. Narcotic pain medication is provided; however, approximately 20% of patients do not require any narcotics after surgery and the average patient might take narcotics for a day or two after surgery and then stop. Overall, this is not an intrinsically painful procedure compared to others. It takes 4 to 6 weeks to heal from a lumbar microdiscectomy. There are some patients in the first week or two after surgery that will have a flare-up of back or leg pain, which can be uncomfortable, but often responds to steroids. This is not a predictor of a poor outcome. If a patient is 6 weeks out from a lumbar microdiscectomy and develops new symptoms or has symptoms that did not resolve with surgery, we believe that we should not blame the symptoms on a flare-up from surgery, but investigate as to whether there is some other source for their persistent symptoms. Although most patients do quite well with a lumbar microdiscectomy, if they have continued symptoms, there is usually a reason for this and often there are other options to treat these symptoms. Approximately 10-15% of patients that have a disc herniation will have another one at the same location whether they have surgery or not. This is because the piece of disc material that ruptured into the spinal canal is only a small percentage of the overall disc and the remainder of the disc still has the ability to rupture additional pieces into the canal. Gratefully, this only occurs in a minority of patients.
Postop Recovery: In our practice, a lumbar decompression or lumbar microdiscectomy is an out-patient procedure. During the surgery, local anesthetic is placed in the skin and in the muscles so that when the patient wakes up, much of their postoperative pain is blocked. This can last between 8 and 24 hours and people are able to ambulate out of the hospital. I tell patients that the skin heals in 1 to 2 weeks unless a patient has a wound healing problem. In this surgery, the muscle is lifted off the spine so that decompression can be performed. It takes 4 to 6 weeks for the muscle to heal back down to the bone. In the first week or two after surgery, because of swelling from surgery, some patients can have a flare-up in the pain in their legs, which we may treat with oral steroids. I expect for patients to be 90% better by 6 weeks postop. People that do office/desk type work will typically return to work between 3 days and 2 weeks after surgery. People that perform physical labor may be off work 6 to 8 weeks.
A lumbar fusion procedure can be performed in many different ways. Some surgeons go through the belly to do this, others go through the back, and some use a combination of both techniques. In our practice, the majority of the time we perform a lumbar fusion through a midline incision in the lower back. We elevate the muscles off the spine just enough to create necessary space to place screws in the bones, which are later connected by rods. We then decompress the nerves, typically going around them to take out the disc. Next, we place a metal box, called a cage, in the disc space. The screws and rods act like a clamp to hold the cage in place. In the cage, and around the cage in the disc space, bone graft material is placed. Over time, the two bones grow together to become one bone as the disc space fuses. There are other techniques used for fusing from the back, including the packing of bone on the back of the spine. We try to employ the least invasive surgical techniques necessary, to decrease blood loss and postoperative pain, while still obtaining a high fusion rate.
Postop Recovery: In our practice, 90% of patients that have a lumbar fusion will either go home the same day or the following day. Patients that are older and live alone and have limited support, are the ones that seem to be in the hospital a few days longer or might require rehab. After surgery, we do not use lumbar braces, as we believe the implants that we place in the spine are strong enough to hold the patients’ bones together without the need for a brace. After surgery, my patients are allowed to walk, do stairs, bend over and twist, although they might be sore doing those things. The volume of activity is less about doing any one thing and more about the volume of it. I encourage gradual physical activity and walking without “overdoing it”. Too much exertion too soon has the potential of working the screws loose before the bones are healed together. In many patients, by 2-1/2 months, the bones are healed together enough that I do not worry about them increasing their activity level. Whether a patient is my best patient or worst patient as far as postoperative recovery is concerned, their activity restrictions are the same, as it simply takes time for bones to heal properly. I do not see a benefit of increasing activity levels until the bones are adequately healed. As with other procedures, the skin heals within a few weeks. The muscles heal in 6 weeks and the bone takes between 2-1/2 to 4 months in the average patient. Even once the fusion is solid, when the patient returns to heavier activities, it is relatively common to be sore for the first month of increased activities, before once again trending in a good direction.
This is a fusion of at least one level in the thoracic spine involving implantation of hardware and the use of bone graft. This procedure is often performed for spinal cord compression or a significant fracture in the thoracic spine.
This is a fusion of at least one level in the thoracic spine involving implantation of hardware and the use of bone graft. This procedure is often performed for spinal cord compression or a significant fracture in the thoracic spine.
This procedure is p performed to treat a compression fracture of a vertebral body in the spine. A balloon is inserted into the bone and then inflated. The void created in the bone is then filled with cement to stabilize the fracture and provide pain relief.
Faqs
Links to Implant Websites
-
https://www.centinelspine.com/prodisc_c.phphttps://www.centinelspine.com/prodisc_c.php
-
https://www.gsurgical.com/products/pedicle-screw.htmlhttps://www.gsurgical.com/products/pedicle-screw.html
-
http://web.orthofix.com/Products/Pages/M6-C-Artificial-Cervical-Dsic.aspx?catid=16http://web.orthofix.com/Products/Pages/M6-C-Artificial-Cervical-Dsic.aspx?catid=16
-
https://www.medtronic.com/us-en/patients/treatments-therapies/cervical/treatment-options/cervical-disc-replacement.htmlhttps://www.medtronic.com/us-en/patients/treatments-therapies/cervical/treatment-options/cervical-disc-replacement.html
-
https://zavation.com/product/zavation-cervical-plate/https://zavation.com/product/zavation-cervical-plate/
-
https://simplifymedical.com/simplify-disc/https://simplifymedical.com/simplify-disc/
-
https://www.indiusmedical.com/https://www.indiusmedical.com/
